
Member Prices
Non-Member Prices
This workshop covers what is known about the etiology and symptoms of IBS, how IBS patients present in clinical practice; IBS in the context of co-morbid panic and agoraphobia, social anxiety disorder, ARFID and depression; formulating appropriate treatment goals and basic cognitive and behavioral strategies for treating IBS, including IBS that is comorbid or secondary to a more serious IBD. Case material reflecting patients along a spectrum of severity is provided for aquisition of new skills and techniques. Application of evidence-based psychotherapies to chronic GI disorders is now referred to as psychogastroenterology.
Post-workshop, participants will be invited to complete a series of reflection questions to help consolidate learning and reduce barriers to applying new knowledge and skills to their clinical practice. (See Bennett-Levy, J., & Padesky, C. A. (2014). Use it or lose it: Post-workshop reflection enhances learning and utilization of CBT skills. Cognitive and Behavioral Practice, 21(1), 12-19.).
Gastrointestinal disorders of all kinds are exacerbated by stress and are also stressful. Irritable Bowel Syndrome (IBS) is a highly prevalent (approximately 10% of the general population but up to 30% of psychiatric treatment seeking individuals) disorder of gut-brain (or central-enteric) interaction that is highly co-morbid with anxiety disorders and depression and shares conceptual overlap with panic disorder, agoraphobia, social anxiety and ARFID. It also leads to considerable disability and distress. Managing these patients effectively requires a good conceptual understanding of the biopsychosocial and cognitive underpinnings of IBS as well as the kinds of avoidance behaviors (both obvious and subtle) that maintain and often exacerbate both symptoms and disability. General CBT skills are essential, but incorporating GI specific phenomena (like bowel control anxiety and fear of food) are also important. There is significant empirical evidence supporting the use of CBT in treating IBS, including multiple RCTs.
Learning Objectives
- What therapists need to know about the etiology, prevalence, symptoms, complications and medical treatment options of both irritable bowel syndrome (IBS) and inflammatory bowel disease (IBD) in order to work effectively with these patients.
- How to develop a case conceptualization that integrates GI disorders with any co-morbid mood or anxiety disorders, including the unique cognitive distortions and behavioral avoidance strategies (especially fear of incontinence and dietary restrictions) that tend to maintain and exacerbate distress and disability in GI disorders.
- How to modify the standard CBT approach to anxiety disorders to treat GI patients effectively, including collaborating successfully with gastroenterologists and considerations about medication.
Anxiety and Depression Association of America
2024 ADAA Webinar: CBT for Chronic Gastrointestinal Disorders-They’re
More Common Than You Think! - Melissa Hunt
Date of CE Release: 10-17-2024
Date of CE Expiration: 10-17-2026
Location: Online















ADAA Continuing Education Credits for Live and On-Demand Programming
Learners complete an evaluation form to receive a certificate of completion. You must participate in the entire activity as partial credit is not available. If you are seeking continuing education credit for a specialty not listed below, it is your responsibility to contact your licensing/certification board to determine course eligibility for your licensing/certification requirement.
Some ADAA professional webinars focused on diversity or cultural competency subject matter are eligible for the Cross-Culture Competency Diversity Credit. If a webinar is eligible for this credit, it will be reflected on your credit certificate.
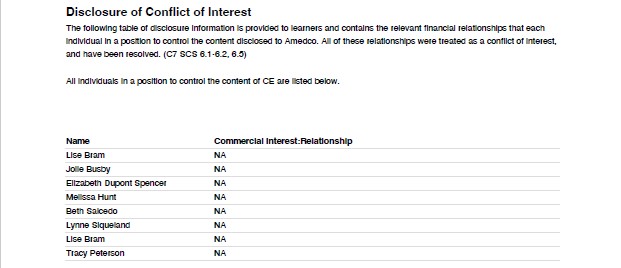
All continuing education credits are provided through Amedco, LLC. Learn more about the CE/CME accreditation information here.